Nursing homes across the country have been facing a financial crisis for years, leading to hundreds of closures throughout the nation. Amid growing financial challenges due to COVID-19, nursing homes are at an even greater risk of shutting their doors.
There have been 550 nursing home closures between 2015 and 2019, and over the past 10 years, more than 440 rural nursing homes have closed or merged according to reports. Residents are forced to uproot their lives to find new care, often hours away from their loved ones.
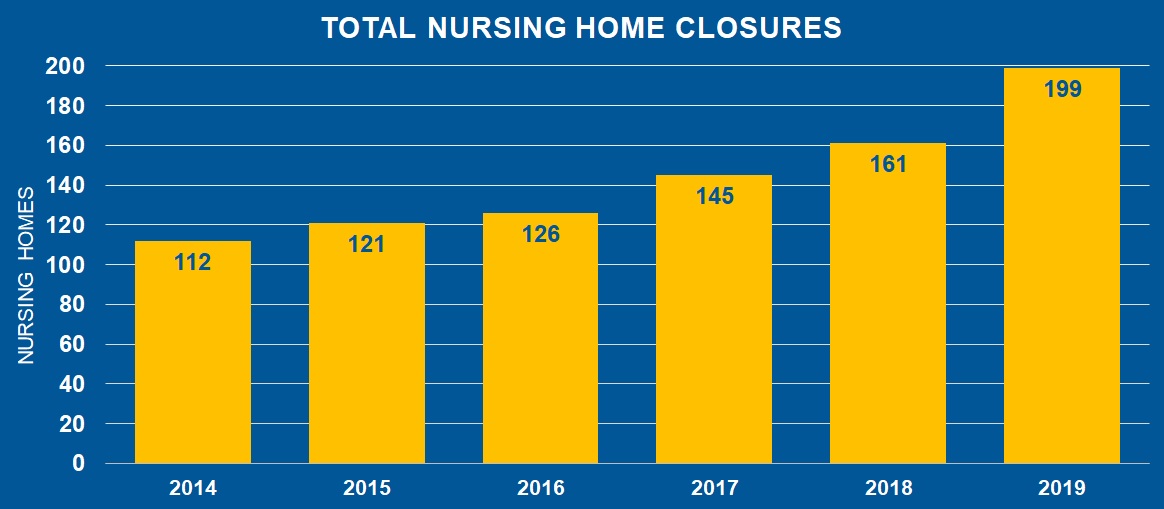
Data compiled by the American Health Care Association and National Center for Assisted Living (AHCA/NCAL) shows that nursing home closures have been increasing since 2014, topping nearly 200 in 2019.
Shortfalls in Medicaid funding are partly to blame. Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long term care services. However, Medicaid reimbursements only cover 70 to 80 percent of the actual cost of care. Low reimbursements rates have forced nursing homes to operate under miniscule budgets and net losses.
These financial strains have only been exacerbated by COVID-19.
Data compiled by the American Heath Care Association and National Center for Assisted Living (AHCA/NCAL) reveal how much nursing home expenditures have increased to fight the pandemic:
- Supplies to fight COVID-19 can increase costs up to 103 percent.
- Labor costs have increased up to 18 percent on average.
- Occupancy is down by nearly 100,000 residents.
- Estimated revenue loss of up to 23 percent, or $57 billion.
- Significant drop in post-acute care patients, which helps many facilities keep their doors open.
Already, COVID-related nursing home closures are becoming an unfortunate reality.
- Sanctuary at the Park in Muskegon, Michigan recently closed down citing “a decline in resident numbers and hospital referrals during the coronavirus pandemic” as the cause of the closure.
- In Providence, Rhode Island, Hallworth House, a nursing home that had been open since 1968, expects to close its doors at the end of August. Dr. Patricia Nolan, chair of the board at the facility said, “The facility had lost more than $1.3 million in the last years while maintaining high standards of care, but the COVID-19 pandemic made it impossible to continue.”
- Family-run Rose Haven Assisted Living in Merrimack, New Hampshire, has been forced to close because of the financial hit they’ve taken due to the pandemic. The community’s administrator, Cindy Gaudreault, said the decision to close was heartbreaking. She added, “Some of my people are still crying. We have a woman who has been with us for 10 years and she is moving out this week. They don’t want to go. This has been their home.”
- Operators of Aperion Care Cairo in Cairo, Illinois are strongly considering closing the facility – the only one in the city – because of the negative impact of the pandemic and lack of funding. According to a 2019 report, Illinois ranks 49th in the country for reimbursement rates.
In order to protect access to long term care for vulnerable seniors, Medicaid reimbursement rates must catch up with the cost of care. Dr. David Grabowski, a professor of health care policy at Harvard Medical School, and Dr. Vincent Mor, a professor at Brown University urged, “Medicaid must begin to pay a higher rate commensurate with the costs of delivering high-quality long-term care to frail older adults.”
With a growing elderly population who have increasing care needs, the need for long term care is evident. Nursing homes need adequate funding and resources in order to provide quality care for our most vulnerable population. It’s time federal and state governments to work toward long-term solutions that will ensure nursing homes remain an option for those who require round-the-clock care.
ABOUT AHCA/NCAL
The American Health Care Association and National Center for Assisted Living (AHCA/NCAL) represents more than 14,000 non-profit and proprietary skilled nursing centers, assisted living communities, sub-acute centers and homes for individuals with intellectual and development disabilities. By delivering solutions for quality care, AHCA/NCAL aims to improve the lives of the millions of frail, elderly and individuals with disabilities who receive long term or post-acute care in our member facilities each day. For more information, please visit
www.ahcancal.org.